Multi-compartment compliance aids - are they ever a good option?
In Pharmacists
Follow this topic
Bookmark
Record learning outcomes
Many pharmacists, when faced with a patient having difficulty taking their medicines, would suggest a multi-compartment compliance aid (MCA) as one of their first recommendations without considering any alternatives. Guidance from the Royal Pharmaceutical Society (RPS) "Improving Patient Outcomes" suggests that this may not always be the best option for all patients and that an MCA should be considered as one intervention amongst many.
Alternative options to an MCA could include:
- Counselling and education of the patient
- Reminder charts that act as a memory aid
- Labels that include large print or pictograms
- Information sheets
- Reminder alarms
- IT solutions such as phone apps
- Simplification of the medicines regime
- Aids for taking medicines such as devices for removing tablets from blister packs or easy open bottles
The RPS recommends that the preferred option is to always supply patients with medicines in original packs and to support the patient in their use for example with the use of large print labels, additional information labels or with counselling. Where patients can safely administer their own medicines they should be encouraged to do so. Where they are unable to self-administer, their carers should be trained to ensure that they can safely administer medication from the original pack.
Assessment of patient needs
It is a common misconception amongst care agencies that their workers are not legally allowed to give medicines from original packs. This misconception has arisen from the widespread use of MCA and the assumption that they are a safer, cheaper and time saving option because carers do not need to identify medicines or record their administration and that an MCA can also help with spot checks of medicines administration.
The end result of this is that some medicines policies do not allow care workers to administer medicines from original packs and it could be considered that the MCA has reduced the carer's skill level. The main disadvantage of carers being unable to administer medication from original packs is that, where medicines cannot be included in an MCA (e.g. inhalers, antibiotics, warfarin, 'when required' drugs and when there are stability concerns) carers may not be aware of or know how to administer them, leading to patients missing doses.
The RPS advises that every patient who is identified as having difficulties with medicines adherence should be assessed using a national multi-disciplinary assessment tool designed to identify, assess and resolve any medicines related issues. This assessment should include a clinical medication review, identification of reasons for non-adherence whether intentional or non-intentional, assessment of suitability of the medicines for inclusion in an MCA and considerations of all of the options to help the patient improve their adherence.
The clinical knowledge of a pharmacist will put them in an ideal position to assist in this assessment process. A national assessment tool has yet to be developed but there are examples of tools currently in use on the RPS website. Both the London Older Peoples Service Development Programme (ref 3) and the NHS Greater Glasgow and Clyde Managing Medicines Guidance (ref 4), available through the RPS website, provide assessment tools that detail patient characteristics such as dexterity, memory, sight, impaired hearing, language problems, literacy problems, learning disabilities, patient beliefs and choices that should be considered during the assessment along with any reasons for poor adherence with medication regimes. They both also suggest methods that can be used to help patients with their medication without the need to use an MCA e.g. large labels, wing top or easy open bottle lids or medication reminder charts.
Where this assessment indicates that an MCA is an appropriate option for the patient then the provision of an MCA must be supported with appropriate information, counselling and a regular review of the patient's ability to use the pack. Each pharmacy and GP practice that provides or requests an MCA should have an SOP in place to ensure that patients receive their medication at the right time each week or month.
Issues with removal from manufacturer's packaging
MCA are associated with an increased risk of dispensing error because of the transfer of medication from the manufacturer's original pack to the MCA. There is also the problem of accurate labelling to ensure that each of the medicines are identifiable and can be easily distinguished from the others. Further issues are that not all medicines are suitable for inclusion in an MCA, due to product stability or incompatibility, or due to complicated dosage regimes. It can cause considerable patient confusion, in patients already struggling with adherence, when different packaging systems are used for medicines that do not fit into the MCA.
In addition, the re-packing of medicines is outside the terms of the manufacturer's marketing authorisation. The use of a medicine 'off licence'results in the responsibility for the stability (and hence safety and efficacy) of the medicine transferring to the prescriber and supplying pharmacist. This is because when the MHRA grant product licences for medicines the impact of the packaging on the product stability is taken into account and as a consequence re-packing the medicine may affect the product's stability and invalidate the product licence.
Medicine-specific issues
Some medicinal products are especially sensitive to water vapour, gases and exposure to light, some or all of which can cause degradation and consequently reduced efficacy of the medicine. A sealed MCA will give greater protection against moisture and atmospheric gases than an unsealed version.
When assessing the suitability of a product for inclusion in an MCA the pharmacist should consider the impact of dispensing into an MCA on the stability of the product.
The packaging used by the manufacturer is a good indication of the stability of the medicine; manufacturers will not use expensive packaging materials like foil or glass unless stability tests have indicated that they are necessary. Similarly desiccants will not be included unless there is a definitive requirement for reducing moisture contact. Dark blisters will indicate the need to protect the medicine from light, whilst coatings on tablets will confer some protection to the product. Sugar coating will give more protection from moisture than film coating whilst specialised coatings can be used to protect against atmospheric gases, moisture and light.
The inclusion of the product on the PSNC special container database is also an indication of stability issues as special container status will only be approved where stability issues are proven. This is not always a definitive guide; for example Prograf is listed in the special container database but is detailed in the PJ article (reference 2) as stable for inclusion in an alternative container with stability data for 3 months at 30°C and 75% humidity.
Effervescent or dispersible formulations and other hygroscopic medicines are unsuitable for dispensing in an MCA because they are highly sensitive to the effects of moisture which will adversely affect product stability.
Medicines administered by the buccal or sublingual route are not suitable for inclusion in an MCA because of the risk of them being swallowed. Cytotoxic medicines should not be included in an MCA because of the risk of topical absorption of the drug if the tablets are touched during the dispensing or administration process. Medicines like glyceryl trinitrate or clomethiazole that are packed in glass bottles should also not be included because of limited stability.
Medicines that are stored in the fridge are unsuitable for inclusion in an MCA unless only the refrigerated medicine is included in the MCA and the complete unit is stored in the fridge. This may complicate administration and lead to further adherence issues. Decisions over supplying controlled drugs in an MCA should be made in the same way as for other medicines with regards stability. But where controlled drugs are subject to safe custody storage requirements, the complete pack will need to be stored in the controlled drug cupboard.
Medicines that are prescribed on a 'when required' basis or medicines where the dose may regularly vary (such as warfarin) should also not be supplied in an MCA due to the practical difficulties associated with medication changes and the issue of waste. Medicines with specific dosage instructions such as bisphosphonates should not be routinely supplied in an MCA but where this is the only option for ensuring adherence the drug could be packed into an individual MCA with guidance on how to take the medication.
The water content of gelatin capsules, both soft and hard, could make them unsuitable for inclusion in an MCA together or with other tablets as the water from the gelatin can move into the other medication causing degradation.
Water movement from gelatin capsules into modified release tablets could alter the release mechanism, and water movement between soft and hard gelatin capsules can cause them to become soft and distorted or brittle. Whilst this information is theoretically correct the impact on the practical use of MCA is unclear and each patient's medication should be considered individually.
Guidance and documentation
There have been very few published reports detailing the stability of medicines in MCA; several articles have been included in the Pharmaceutical Journal, although the most recent article was published in 2006. This article titled “How stable are medicines moved from original packs into compliance aids” (ref 2) lists individual drugs and their brands names along with appropriate recommendations on their suitability for inclusion in the MCA. Pharmacists can also access individual SPCs to obtain information on factors that may affect stability.
In an attempt to support pharmacists to make informed decisions over the stability of medicines in an MCA, the UKMi developed an open access online database of stability information. This database provides information on the stability of medicines within a MCA, using a traffic light system to indicate any potential risk. Red indicates the product is unsuitable for inclusion in an MCA whilst green indicates the product is suitable, and amber indicates different levels of risk alongside actions that can be taken to mitigate this risk. This database can be accessed at https://www.sps.nhs.uk/
Numark members can contact Information Services for advice regarding the suitability of medicines for inclusion in a MCA.
As re-packaging medicines into an MCA can affect their stability and as there is no comprehensive data source on the stability of medicines in an MCA the RPS recommends a maximum expiry date of eight weeks for medicines dispensed into a sealed MCA, whilst for an unsealed MCA a seven day expiry should be applied (ref 1).
Documentation should be kept to provide a comprehensive audit trail of the care provided to patients where medicines are supplied in an MCA. This supporting documentation should include patient assessment documents, reasons behind decisions to include or exclude medicines from an MCA, records of medication changes and who initiated the requests for change, records of medication collected or delivered and where appropriate details of carers alongside other clinically relevant information.
Advice for patients and carers
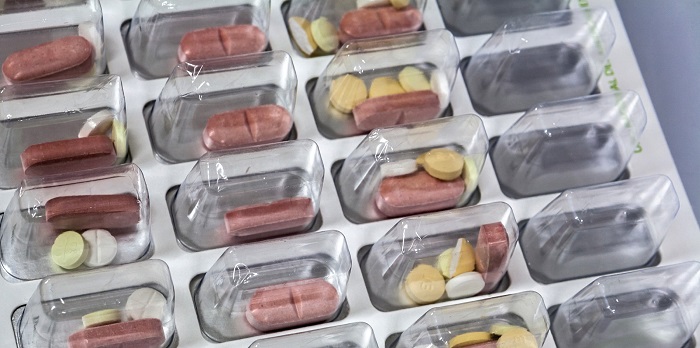 Patients or their carers supplied with an MCA should be counselled about keeping the compliance aid out of the reach of children as the packaging is unlikely to be child resistant and also to store it in a cool dry place and out of direct sunlight.
Patients or their carers supplied with an MCA should be counselled about keeping the compliance aid out of the reach of children as the packaging is unlikely to be child resistant and also to store it in a cool dry place and out of direct sunlight.
Where medication changes are required, patients should be advised to contact the pharmacy and to not attempt to change the packs themselves. This may generate problems for the pharmacy associated with adding or removing medicines from the pack mid-cycle. Probably the safest and most effective option would be to agree locally with the prescriber to make medication changes at the end of the cycle, although the practicalities of this would need to be assessed on an individual basis.
Advice should also be given over what to do if they spill medicines from the compliance aid or the medicines move inside the aid. Patients and carers should be advised to return the pack and medicines to the pharmacy rather than try to put the medicines back themselves. The pharmacist may need to arrange for an additional supply of medication to cover any loss.
Patients, carers and healthcare professionals will benefit from including an accurate description of the appearance of each medicine within the MCA. As generic medicines vary in colour, size and shape it is important to check these descriptions with each supply to ensure the description is accurate. This description can help to maintain the independence of the patient in allowing them the decision over whether to take a particular medicine or not, it will also avoid confusion for both the patient and their carer if they try to identify particular medicines. In addition it may also help to avoid a delay in administration of medicines where patients are transferred to a different care provider as carers are required to be able to identify medicines before administration.
Legally each medicine dispensed into an MCA requires a dispensing label to be attached to the package. The MCA should therefore have sufficient space for all of the medicines to be labelled and there should be no risk of the labels being separated from the MCA.
In addition it is a legal requirement that each medicine in the MCA should be supplied with a patient information leaflet (PIL) each time an MCA is supplied. Whilst it is acknowledged that patients and carers should have access to a PIL there are practical issues associated with the supply of a PIL with each seven day supply. The RPS recognise that with consent an agreement can be made between the patient and pharmacist over sensible options for the supply of a PIL, for example supply every four weeks or 28 days. Pharmacists are advised to document any agreement on the patient's notes or PMR as provision of a PIL remains a legal requirement and careful consideration should be made of the possible consequences of not supplying a PIL each time, for example a supply without a PIL being considered a dispensing error.
Practical considerations
From a practical perspective medication should never be dispensed into an MCA in foil strips or blisters as there have been cases where patients have swallowed their medication and foil together causing gastro-perforation. This is not a solution that allows medicines with limited stability to be included in an MCA.
The hygiene and risks of contamination with dust or dirt during dispensing as well as previously dispensed medication where parts of the MCA are re-usable must be considered when preparing an MCA. If any part of the MCA is not disposable it should be thoroughly cleaned before re-use in line with the advice of the manufacturer.
Patients who live alone may benefit from a delivery service but the benefit of this must outweigh the potential risks of not seeing the patient on a regular basis to allow for review of adherence and safe use of their medication. This potential risk could be overcome by the provision of home visits to house-bound patients to carry out Medicines Use Reviews.
The frequency of supply of the pack should be agreed between the pharmacist, patient and prescriber. This agreement should be made after considering the stability of medicines, the risks associated with the supply of multiple packs and the possibility of medication changes necessitating re-dispensing and re-supply of amended packs.
The PSNC has advised that where pharmacists receive a prescription for 28 days treatment for a patient who is assessed to need their medication in an MCA that they should prepare either a 28 day MCA or four, seven day MCAs on one occasion.
Where the patient's medication changes mid-month there is no obligation on the pharmacy to amend dispensed medication and any alteration should be authorised by a new prescription with previously dispensed medication being discarded. The prescriber may decide to advise the patient to remove and not take a particular medication if it is easily identifiable by the patient but the risks inherent in this practice mean we would not advise it. Where a new medication is started midway through a cycle it is advised that a complete new pack is dispensed rather than issuing a separate pack containing only the new medication as this could cause confusion resulting in the medications not being taken as prescribed. Where patients are having frequent medication changes prescribers could be advised to issue seven day prescriptions to minimise waste. (Ref 5)
Summary
In summary, the guidelines issued by RPS encourage pharmacists to formally review patients to assess adherence and to consider all of the options for improving compliance without simply opting for an MCA. They also advocate consideration of the suitability of medicines for inclusion in the MCA. It is hoped that this guidance will act as a tool to enable pharmacists to refuse to supply an MCA where they feel it is not necessary or appropriate. By reviewing these guidelines we aim to support members on the issues surrounding supply of medicines in MCAs.
The supply of an MCA should not be the default option for patients with adherence issues, but just one option in a range of possible actions. Pharmacists should be able to explain the appropriate use of MCAs to patients, carers and healthcare professionals and engage them in discussions over alternative options to consider.
Until change is agreed at a national level this report from the RPS can be used as a guide for pharmacists in the decisions they make over provision of medicines in MCA packs.
References
Ref 2. “How stable are medicines moved from original packs into compliance aids” PJ vol. 276 21/1/2006
Ref 3. London Older Peoples Service Development Programme
Ref 4 NHS Greater Glasgow and Clyde Managing Medicine Guidance
